Doctor-Led Aesthetic Medicine
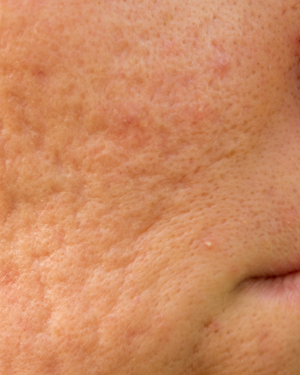
Acne scarring is a long-lasting change in skin texture that can develop after inflammatory acne has healed. When acne affects the deeper layers of the skin, it can disrupt the normal collagen support structure. As the skin repairs itself, this healing process does not always occur in a balanced way.
If too little collagen is produced during healing, indented or pitted scars can form (atrophic scars). In other cases, the skin mounts an overactive repair response and produces excess collagen, leading to raised scars (hypertrophic scars). In both situations, the result is uneven skin texture that can remain long after active acne has settled.
Acne scars are different from the temporary marks that often follow a breakout. Flat red or brown marks, known as post-inflammatory erythema or hyperpigmentation, are colour changes rather than true scars and often fade gradually with time and appropriate skincare. True acne scars involve a structural change within the skin and usually require targeted treatment to significantly improve texture.
Acne scarring develops as part of the skin’s healing response to inflammation. Understanding why scars form helps explain why early acne treatment and appropriate scar management are so important.
The more inflamed a breakout becomes, the higher the risk of scarring. Cystic and nodular acne develop deep within the skin and can cause significant damage to the surrounding tissue. As these lesions heal, the normal collagen framework is often disrupted.
Picking, squeezing, or repeatedly touching spots increases inflammation and can push bacteria deeper into the skin. This creates additional trauma and significantly raises the risk of scarring.
The longer acne remains active and untreated, the greater the chance of scarring. Ongoing inflammation over months or years causes cumulative damage to the skin’s support structures.
Some people are naturally more prone to acne scarring than others. A family history of acne scars can increase your own risk. Genetics also influence how your skin produces and remodels collagen during healing.
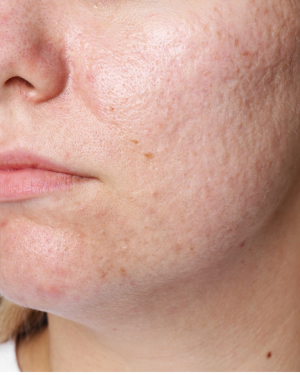
Not all acne leaves scars, but when inflammation runs deeper in the skin it can sometimes leave lasting changes in texture. Understanding the type of acne scarring present is an important first step, as different scar patterns often need different treatment approaches.
These are the most common type of acne scars and appear as indentations in the skin caused by loss of collagen during healing. They are usually divided into three main types: ice pick, boxcar and rolling scars.
Ice pick scars are the most common type of atrophic acne scar. They appear as narrow, deep indentations that extend into the skin, often looking like enlarged pores or small puncture marks. Although usually less than 2 mm wide, their depth can make them more challenging to treat.
They are often seen in areas where the skin is thinner, such as the forehead and upper cheeks, and tend to respond best to treatments that work deeper within the skin rather than surface resurfacing alone.
Boxcar scars account for around 20–30% of atrophic acne scars. They appear as round or oval depressions with clearly defined edges and a relatively flat base, giving the skin a pitted appearance similar to chickenpox scarring. They are usually shallow to medium in depth and often respond well to collagen-stimulating treatments.
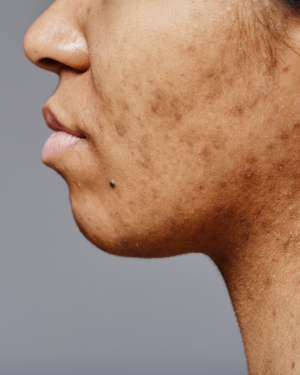
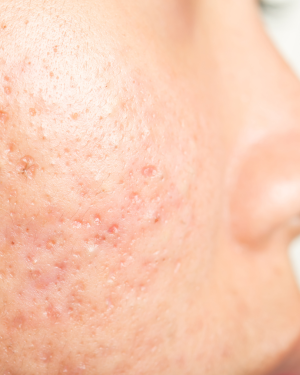
Rolling scars make up around 15–25% of atrophic acne scars. They appear as wider depressions with gently sloping edges, giving the skin an uneven or wave-like texture. They develop when fibrous bands form beneath the skin, pulling the surface downwards, and often respond best to treatments that help stimulate collagen and release this tethering.
Hypertrophic and keloid scars are raised scars that sit above the level of the surrounding skin, unlike atrophic scars which appear as indentations. They develop when the skin produces excess collagen during healing, resulting in thicker areas of scar tissue. These scars are more common on the jawline, chest and back, and often require a different treatment approach from indented scars.
Most people with acne scarring have a mixture of different scar types rather than just one. It is common to see ice pick, boxcar and rolling scars affecting different areas of the face at the same time. Because each type responds differently to treatment, careful assessment is essential when deciding the best approach.
Real Results
Swipe to reveal the transformation. See the remarkable results our patients have achieved.
Dr Rachel answers your common questions about acne scarring
Over-the-counter creams containing ingredients such as retinol or vitamin C can help with mild surface discolouration, but they usually contain lower concentrations of active ingredients. Skincare is important, but it needs to be carefully chosen and used consistently to make a real difference. More established acne scarring involves deeper structural changes that topical products alone cannot reach. Treatments such as medical microneedling can help stimulate collagen to improve skin texture, while chemical resurfacing supports skin renewal and smoother skin. The most effective approach usually combines the right homecare with appropriate in-clinic treatments. Skincare does much of the daily work, but in-clinic treatments can help create the changes that skincare alone cannot achieve.
Acne scars do not spread, but their appearance can become more noticeable over time. Natural collagen loss and reduced skin elasticity can make existing scars appear deeper, while sun exposure can worsen surrounding pigmentation and make scarring more visible. Early intervention with collagen-stimulating treatments such as medical microneedling or regenerative treatments like JULÄINE™ can help support skin structure while your skin still has good healing capacity. Addressing any associated pigmentation early can also help prevent discolouration from becoming more persistent. Treating scars earlier often allows for better improvement than waiting until collagen loss progresses.
Yes, and a combination approach often delivers the best results. Treatments such as medical microneedling can be combined with regenerative treatments like polynucleotides to support both collagen production and skin repair. If scarring is accompanied by uneven skin tone, chemical resurfacing can help address pigmentation while other treatments focus on improving texture. Where there are also concerns about overall skin quality, regenerative treatments such as JULÄINE™ may be considered to support collagen strength alongside scar-focused treatments. Treatment plans are carefully planned to combine and sequence treatments safely for the best long-term outcome. Often the best results come from improving the overall health of the skin, not just treating the scar itself.
Treated scars do not return. Once collagen has remodelled and scar tissue has improved, those changes are long-lasting. However, new breakouts in the future can lead to new scarring, which is why it is important to have active acne well-controlled before starting scar treatment and to maintain a good skincare routine afterwards. I may also recommend a longer-term maintenance approach to support your results, which can include periodic skin treatments or collagen-supporting treatments such as JULÄINE™ where appropriate. The goal is not just improvement, but helping your skin stay strong enough to hold those improvements.
I am always happy to help. Please get in touch.